As promised, we’re back with more about Regenerative Medicine. Our first profile is on Organogenesis, a company based in Canton, Massachusetts, who is at the forefront of the field. Their website states that “in the future, regenerative medicine technologies may deliver neural regeneration, islet cells for diabetes, and more substantial heart repair.” For Organogenesis, this process starts with healing chronic wounds.
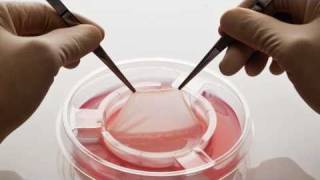
Organogenesis has a product on the market called the Apligraf. The Apligraf mimics human skin to kick-start the healing process. Imagine living for years with an open wound—if you last this long without having to lose your limb that is. Organogenesis’ Apligraf can save the lives of people doing just that, it can save limbs and lives with the simple regeneration of skin cells. The new skin-like graft is created from donated foreskin from circumcision. That may sound weird, but since the Apligraf was developed it has taken twelve donated foreskins and made enough cell lines to create half a million Apligrafs. They take the foreskin cells, break them down, and then fibroblasts and keratinocytes, a bottom and top layer respectively, are used to create a remarkably skin-like bilayer graft.
This forty-four square centimeter cell culture can be applied to diabetic foot ulcers as well as venous leg ulcers, which makes it unique from any other similar product. It is designed to be applied to the patient’s wound and using the young and healthy cells in the Apligraf stimulate the body to make cells and heal itself. This revolutionizes the healing process for people with chronic wounds and can give them their lives back!
Want to know more about what else Organogenesis is doing? Stay tuned until our next post when we talk about the rest of their technology! Let us know what you think so far at @TRA360!